
| Blogs and publications on this website are independent of any involvement by medtech companies or diabetes related charities. To ensure there is no bias, we do not accept any products, freebies or other material from any medtech provider. All materials are copyright©️Love My Libre Ltd. |
***
We often hear reference to ‘hormones’ in relation to diabetes and there seems to be an underlying assumption that we know and understand the terminology and how this affects us. But I for one, will admit that I don’t always know what this means for me as a type one.
To better understand how hormones affect diabetes, this blog sets out to identify the seven main hormones and their impact on our day-to-day management.
Let’s start with asking, what are hormones?
Hormones are naturally occurring chemicals produced in one part of the body that provide an internal communication system between cells in other parts of the body. They tell the cells in our body and organs what to do.
So, which hormones will affect my diabetes?
Insulin
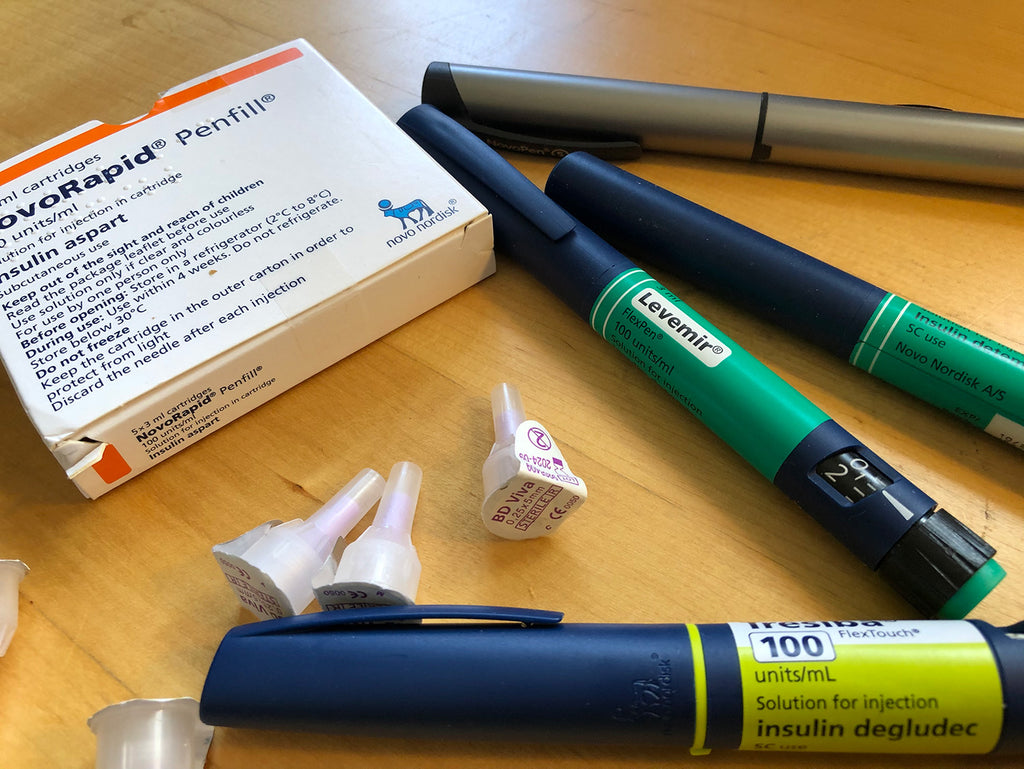
Insulin is a hormone that is naturally produced in the pancreas but as you’ll know, having an autoimmune disease means that our bodies are fighting and destroying the beta cells that produce insulin and we therefore need to inject insulin through multiple daily injections (commonly referred to as MDI) or though infusion using a pump.
Life for a type one requires insulin and in some ways it’s as simple as that! This is also true for other conditions too where the body is insulin resistant or intolerant and can’t process glucose properly. Insulin is vital to control the use of glucose and fat in our blood and cells without which we risk developing ketones leading to DKA (see below).
As we can’t produce our own insulin, we use one manufactured to best replicate the function usually performed by our pancreas, the organ responsible for releasing insulin and glucagon into our cells for use as energy. Insulin helps cells absorb glucose from the blood and store it for later use. DSNs often describe it as a “key” to unlock our cells.
A lot of effort goes into calculating how much insulin we should put into our bodies, usually based on carb counting, but as well as other hormones playing a part, it’s been recognised that there are also over 42 other factors which affect our levels at any time. It’s not surprising that matching the insulin your body needs to what to input is an extremely difficult equation to balance.
|
Ketones are an alternative source of energy produced by the liver. However, high levels of ketones can lead to DKA (diabetic ketoacidosis), a potentially dangerous condition requiring emergency medical treatment.
|
Glucagon
Glucagon performs the opposite function to insulin. Where insulin helps to reduce levels of glucose in the blood, glucagon’s role is to increase glucose levels. Glucagon enables glucose stored in the body to be released into the blood so it can move around and be used for energy.
Glucagon controls glucose and ketone production in our liver and this is generally released by eating protein, when the body is hypoglycaemic and when we exercise, enabling the body to maintain a balanced ‘blood sugar’. Glucagon comes from breaking down starch stored in the liver.
 An injection of Glucagon is sometimes used as an emergency means to trigger the liver to release glucose for energy in the event of a severe hypo.
An injection of Glucagon is sometimes used as an emergency means to trigger the liver to release glucose for energy in the event of a severe hypo.
Important point: Glucagon is ineffective at raising blood sugar when dealing with a hypo if you have been drinking alcohol. This is because the liver’s function to detox the body of alcohol takes precedence, and it is unable to break down glucagon at the same time.
Adrenalin

When we are stressed, the body triggers the fight-or-flight response, and the hormones adrenalin and cortisol are released. The effect of adrenalin is to prepare the body for this response - to flee or face the battle.
In a stressful situation you may feel your heart racing, you start to get sweaty or sometimes dizzy, your blood pressure increases, the pupils of your eyes enlarge and the airways in your lungs expand, altering the body’s ability to process food and function efficiently. This is so that blood glucose levels are maximised for brain functionality.
Adrenalin acts fairly quickly, around 2 to 3 minutes of a stressful event and can quickly cause hyperglycaemia. It could be the reason why a horizontal trend arrow suddenly changes direction, to show as a vertical arrow upwards.
Adrenalin, also known as Epinephrine, stimulates the liver to produce glucose and actively release and breakdown fat. This will travel into the liver to be converted into ketones and glucose.
Adrenalin can trigger the release of glucagon that can raise glucose levels as a response to a hypo.
Cortisol
Cortisol is a steroid hormone that regulates many processes in the body including our metabolism and immunity. It can make you more alert, and we generally produce more in the morning with levels falling throughout the day.
Cortisol plays an important role in the body’s response to stress and extra cortisol may be released to help the body to respond to particularly stressful situations.
Cortisol makes muscle and fat cells resistant to insulin so to increase the production of glucose from the liver. Cortisol generally acts as a counterbalance to insulin, however in stressful circumstances cortisol levels can increase such that the body is much more resistant to insulin.
Extra insulin may be needed to control blood sugar levels. This can sometimes feel like we’re “injecting water” as insulin appears to have less effect than usual.
Melatonin

Melatonin is a hormone associated with regulating the body’s rhythm and particularly the daily cycle of being awake and sleeping, sometimes referred to as circadian cycle of 24 hours. It has a significant effect on our body clock and many aspects of our health.
The production of Melatonin is stimulated by darkness and your body will naturally make more of it during the night. In contrast, light suppresses its activity during the day.
It can also be disrupted by a number of other factors, such as excessive light during the night, too little light during daytime, changing time zones, and night work.
Melatonin is also involved in other body cycles, including menstruation, so may account for other effects on glucose levels at different stages of this cycle too.
Amylin
Amylin is a hormone that is produced by the pancreas and released at the same time as insulin, but in smaller quantities. This hormone works to suppress the body from producing glucagon after eating which would otherwise raise ‘blood sugar’ levels. By blocking the release of glucagon, amylin slows down the process of the stomach emptying and curbs our appetite for more food.
The overall effect of Amylin is that it prevents blood glucose levels from getting too high when glucagon is not needed, however this also means that it can prevent the release of glucagon when blood sugar levels are low, leading to hypos which may have a more serious effect.
Growth hormone

Growth hormone is released from the pituitary gland, part of the brain. It functions in a similar way to cortisol and will work to counterbalance the effect of insulin on fat and muscle cells. High levels of growth hormone levels can cause insulin resistance.
Summary
Hormones are part of an internal communication system that tells the cells in different parts of our body what to do. As people with diabetes, we are concerned with 7 types of hormones[1] in particular that have a substantial effect on our ability to balance our glucose levels and manage our diabetes.
In people without diabetes, insulin and glucagon work together to keep blood glucose levels in balance, whereas those with diabetes are well aware of the roller coaster ride when there’s an imbalance between these two hormones. Other hormones play important roles too and the exact correlation and interactions between the different hormones and blood glucose levels is not fully known, making the task of diabetes management all the more difficult. For now, we rely on the hormone of insulin as being vital to our everyday life.
[1] There are other hormones to the 7 identified here, but for brevity they are not covered in this article.
💛💛💛
Disclaimer
Love My Libre is not associated or affiliated with Dexcom, Abbott or FreeStyle Libre. Content here and on our website www.lovemylibre.com does not constitute medical advice or replace the relationship between you and healthcare professionals nor the advice you receive from them.
The author of this blog has type 1 diabetes and uses the FreeStyle Libre 2 which is provided on NHS prescription.
FreeStyle Libre is a registered trademark of Abbott Diabetes Care Inc.
Dexcom and Dexcom G6 are registered trademarks of Dexcom Inc.





Leave a comment (all fields required). Please note, we are unable to respond to individual comments posted here.